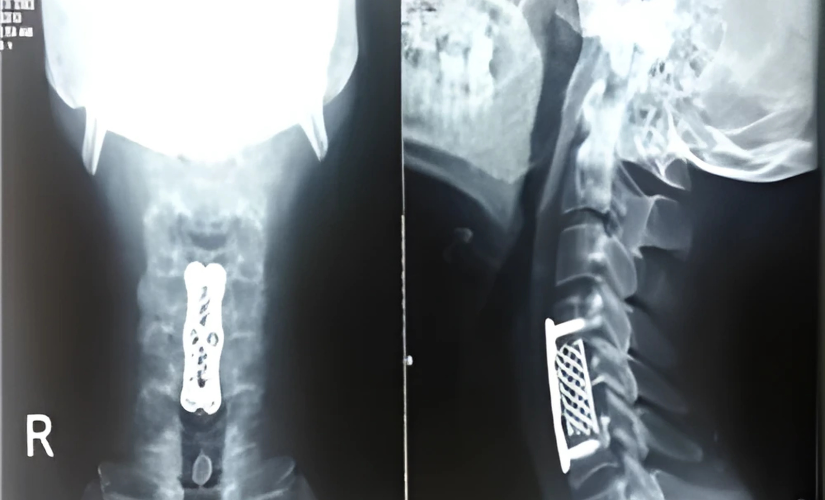
Cervical Disc Disease
Diagnosis primarily involves an MRI scan to evaluate the extent of disc damage and spinal cord involvement. Surgery is generally considered only when nonsurgical treatments fail to provide relief or when neurological symptoms worsen. The most common surgical approach is performed from the front (anterior) of the neck. This procedure involves removing the entire affected disc and replacing it with a spacer. The spacer can be the patient’s own bone, a PEEK cage, a mesh cage with plates, or an artificial disc. The success rate of this surgery is very high.
Surgical Details and Outcomes
The anterior cervical discectomy involves a small incision in the front of the neck to access and remove the damaged disc. The spacer maintains spinal stability and helps restore normal motion. Patients typically experience significant pain relief and improved neurological function after surgery. Recovery varies but is generally favorable, with a focus on gradual rehabilitation and lifestyle modifications to support long-term spine health.
Frequently asked questions
Neck pain, shoulder pain, arm weakness, numbness, and in severe cases, difficulty moving legs due to spinal cord compression.
MRI is the best imaging technique to assess disc degeneration and nerve or spinal cord involvement.
Surgery is considered when conservative treatments fail or when neurological signs like weakness or numbness progress.
Anterior cervical discectomy and fusion (ACDF) with various spacer options, including artificial discs, is the most common.
Surgery has an excellent success rate in relieving pain and restoring neurological function.